Connect With Us

What Is Tarsal Tunnel Syndrome?

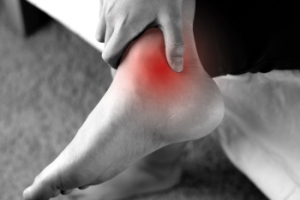
Tarsal tunnel syndrome is a condition caused by compression of the posterior tibial nerve as it passes through the tarsal tunnel near the ankle. This nerve entrapment can result from injury, swelling, flat feet, or medical conditions like arthritis or diabetes. Symptoms include tingling, burning, numbness, or shooting pain in the ankle, heel, or sole of the foot. Risk factors include repetitive motion, improper footwear, and structural foot problems. A podiatrist can diagnose the condition through physical examination and testing, then recommend treatments, such as orthotics or anti-inflammatory care. If you are experiencing these symptoms, it is suggested that you consult a podiatrist for expert evaluation and a plan to restore foot comfort and function.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact Tanisha Richmond, DPM of Richmond Foot & Ankle, LLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please contact our office located in Dayton, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Treating Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which the tibial nerve, located in the tarsal tunnel in the foot, is compressed. The tibial nerve can become compressed from injury, such as an ankle sprain, flat feet, and lesions. Arthritis, diabetes, and varicose veins can also cause swelling and thus result in nerve compression.
Symptoms of tarsal tunnel syndrome include several different sensations in the sole of the foot, inside the ankle, and around the tibial nerve. These sensations include shooting pains, numbness or reduced sensation, pins and needles, burning, and tingling. Symptoms tend to worsen with greater activity to the area. In rare and severe occasions, this can change the muscles in the foot.
If you suspect you have tarsal tunnel syndrome, you should consult with your podiatrist. He or she will examine your medical history to see if you have a history of diabetes, arthritis, or flat feet. They will also check to see if you have suffered an injury to the area recently. An electrical test will be conducted to check if the nerve has been damaged. A simpler Tinel’s Test might also be used. This includes simply tapping the nerve to create a sensation. An MRI scan of the area may also be used.
Treatments vary greatly for tarsal tunnel syndrome. Treatments include both nonsurgical and surgical options depending upon the severity of the condition. Nonsurgical options include anti-inflammatory medication and steroid injections to the area. Orthotics, such as a splint or brace that immobilizes the foot, is another noninvasive option. For those with flat feet, custom shoes can be made to offer better foot support. Surgical options include a tunnel tarsal release, in which an incision is made behind the ankle down to the arch of the foot. This releases the ligament and relieves pressure off the nerve. Some doctors use a more minimally invasive surgery, where smaller incisions are made in the ankle and the ligament is stretched out.
If you are suffering from painful sensations in your foot, see a podiatrist who can determine if you are experiencing tarsal tunnel syndrome. Tarsal tunnel syndrome that is left unchecked can cause permanent nerve damage to the foot.
Broken Toes and the Role of a Podiatrist

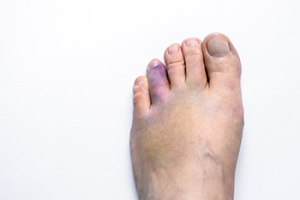
A broken toe is commonly caused by trauma, such as stubbing the toe, dropping a heavy object, or sports injuries. Symptoms include pain, swelling, bruising, and difficulty walking or wearing shoes. In some cases, the toe may appear deformed. Risk factors include weak bones, high-impact activities, and poorly fitting footwear. If left untreated, a broken toe can lead to improper healing and long-term discomfort. A podiatrist can assess the severity of the fracture, provide appropriate treatment, prescribe protective footwear, and ensure proper healing. If you suspect a broken toe, it is suggested that you seek care from a podiatrist who can provide an accurate diagnosis and treatment..
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact Tanisha Richmond, DPM from Richmond Foot & Ankle, LLC. Our doctor will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
- Throbbing pain
- Swelling
- Bruising on the skin and toenail
- The inability to move the toe
- Toe appears crooked or disfigured
- Tingling or numbness in the toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions, please feel free to contact our office located in Dayton, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
Arthritis Can Cause Pain in the Feet and Ankles
Orthotics Can Support Foot Health In Charcot Marie Tooth Disease

Charcot Marie Tooth disease affects the nerves and often leads to muscle weakness and structural changes in the feet. As arches collapse or toes begin to curl, walking can become more difficult and painful. Orthotics play a key role in managing these changes. They help support the foot, improve balance, and reduce the risk of falls or pressure injuries. Custom orthotics can also help slow the progression of deformities by providing better alignment and cushioning. However, their effectiveness depends on how consistently they are worn. Regular use and follow up with a podiatrist ensure that the fit remains correct as the condition evolves. If you or someone you know has been diagnosed with Charcot Marie Tooth disease and is experiencing changes in foot shape or stability, it is suggested that you see a podiatrist for a discussion on how custom orthotics can help you.
Custom orthotics can make a remarkable difference in daily comfort and mobility by supporting the feet in their most natural and balanced position. Because the feet form the foundation for the entire body, any imbalance can affect not only how a person walks, but also how the knees, hips, and spine align. Over time, this can lead to fatigue, pain, or reduced movement. Custom orthotics are designed to restore stability and promote proper alignment, which can transform the way a person feels and functions throughout the day.
People who wear custom orthotics often experience improved posture, less joint strain, and greater endurance during work, exercise, and leisure activities. The support they provide helps relieve chronic discomfort from conditions such as plantar fasciitis, flat feet, and heel pain, while also reducing the risk of future injuries. For those who stand for long hours or engage in sports, orthotics can make movement smoother and more efficient, allowing the body to perform at its best without unnecessary stress.
Each pair of custom orthotics is created after a detailed evaluation of foot structure, gait, and pressure distribution. By addressing each person’s unique needs, they offer comfort and confidence with every step.
If you are experiencing ongoing foot discomfort or fatigue, it is suggested that you contact our office for more information or to make an appointment.
If you have any questions, please feel free to contact our office located in Dayton, OH .
Investing in Custom Orthotics Means Investing in Foot Health
Custom orthotics offer a tailored approach to foot health, providing a host of benefits that extend far beyond conventional shoe inserts. One of the primary advantages lies in their ability to address specific biomechanical issues. Unlike off-the-shelf inserts, custom orthotics are crafted based on an individual's unique foot structure, gait, and any existing foot conditions.
The personalized design of custom orthotics ensures optimal support for the arches, promoting proper alignment and distributing pressure evenly across the feet. This can be particularly beneficial for individuals dealing with issues such as overpronation or underpronation, as custom orthotics help correct imbalances that may lead to discomfort or injury.
Beyond biomechanics, custom orthotics can alleviate a range of foot problems, including plantar fasciitis, bunions, and metatarsalgia. They provide targeted relief to areas under stress, reducing pain and inflammation. Additionally, for those with specific medical conditions like diabetes, custom orthotics can play a crucial role in preventing complications associated with poor foot health.
Comfort is another key aspect of custom orthotics. By accommodating the unique contours of an individual's feet, these inserts enhance overall comfort, making daily activities more enjoyable. Whether for athletes looking to optimize performance or individuals seeking relief from chronic foot pain, custom orthotics offer a versatile solution.
Investing in custom orthotics is an investment in long-term foot health. They not only provide immediate relief but also contribute to the prevention of future issues. With the ability to seamlessly integrate into various types of footwear, custom orthotics empower individuals to prioritize foot comfort without compromising on style. In essence, custom orthotics are a personalized prescription for happy, healthy, and pain-free feet.
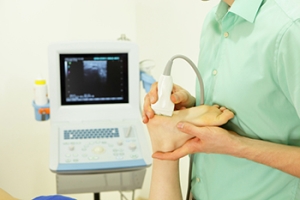
Using Ultrasound to Diagnose Foot Pain in Kids and Teens

When children or teens have foot pain, finding the exact cause is not always easy. Sometimes the pain comes from muscles, tendons, or small injuries that are hard to see with the eye alone. In these cases, ultrasounds can be a helpful tool. It uses sound waves to create real-time images of soft tissues in the foot and ankle. This allows doctors to check for inflammation, tears, or other problems without needing radiation. A problem-based approach means the ultrasound is used to look at specific areas where pain is reported, helping to pinpoint the source. This can lead to faster and more accurate treatment, especially when the pain is not clearly linked to a single injury. If a child has ongoing foot pain that does not improve, it is suggested that you see a podiatrist who may recommend ultrasounds to better understand the issue.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Tanisha Richmond, DPM from Richmond Foot & Ankle, LLC. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Dayton, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Pain
Our feet are arguably the most important parts of our bodies because they are responsible for getting us from place to place. However, we often don’t think about our feet until they begin to hurt. If you have pain in your feet, you need to first determine where on the foot you are experiencing it to get to the root of the problem. The most common areas to feel pain on the foot are the heel and the ankle.
Heel pain is most commonly attributed to a condition called plantar fasciitis. Plantar fasciitis occurs when the plantar fascia, which is the band of tough tissue connecting the heel bone to the toes becomes inflamed. Plantar fasciitis pain is usually worse in the morning, and it tends to go away throughout the day. If you have plantar fasciitis, you should rest your foot and do heel and foot muscles stretches. Wearing shoes with proper arch support and a cushioned sole has also been proven to be beneficial.
Some common symptoms of foot pain are redness, swelling, and stiffness. Foot pain can be dull or sharp depending on its underlying cause. Toe pain can also occur, and it is usually caused by gout, bunions, hammertoes, ingrown toenails, sprains, fractures, and corns.
If you have severe pain in your feet, you should immediately seek assistance from your podiatrist for treatment. Depending on the cause of your pain, your podiatrist may give you a variety of treatment options.
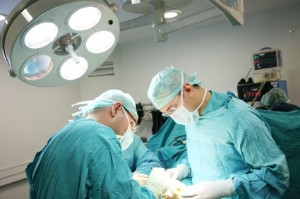
All About Ankle Ligament Surgery

Ankle ligament surgery may be needed when ligaments in the ankle have been torn or overstretched due to injury. The ankle is made up of three joints, and its stability depends on ligaments that connect bone to bone. When these ligaments are severely damaged, surgery may be the only way to restore support. Anatomic reconstruction is an option that involves tightening or repairing the original ligament using tissue from the same area or from a donor. Another method, called peroneal substitution, uses a nearby tendon to replace the damaged ligament, though this may affect long-term function. Other risks of ankle ligament surgery include infection, nerve injury, bleeding, and delayed healing. Recovery can take up to six months and usually includes a period of limited mobility, followed by gradual return to weight-bearing activities. If you have torn or ruptured an ankle ligament, it is suggested that you schedule an immediate appointment with a podiatrist for an exam and prognosis on the type and level of surgery that may be involved, if needed.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact Tanisha Richmond, DPM of Richmond Foot & Ankle, LLC. Our doctor will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions, please feel free to contact our office located in Dayton, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.